Preventing calcification of bioprosthetic heart valves
A defective heart valve is the second most common form of heart disease. Most cases involve a narrowed aortic valve, but often the mitral valve can also be affected. Prostheses significantly increase the life expectancy of those with the disease. While bioprosthetic heart valves have some advantages over me-chanical ones, they can become calcified relatively quickly, limiting the length of their useful life. A team of researchers at the Fraunhofer Institute for Ceramic Technologies and Systems IKTS is attempting to prevent such calcification with a new chemical pretreatment of the bioprostheses.
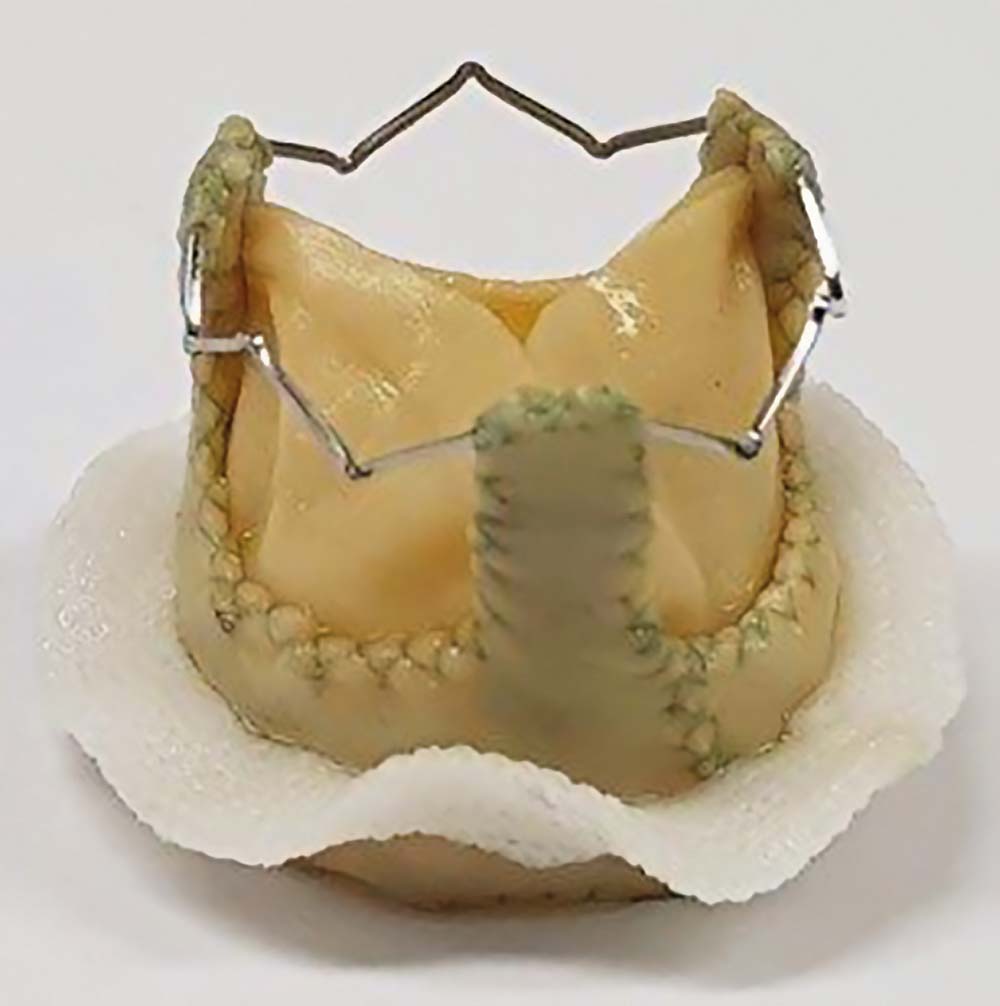
If a heart valve stops opening and closing properly, it often needs to be replaced with an artificial one. We are currently seeing a trend towards biological valves because they do not require the patient to take blood-thinning medications, such as Marcumar. Mechanical valves, on the other hand, require life-long treatment with anticoagulants. The downside of bioprostheses, which are made either from pig aortic valves or from bovine pericardial tissue, is that they normally only last up to 15 years because of the effects of calcification and material fatigue on the proper functioning of the valve leaf-lets. Crystalline hydroxyapatite forms deposits on the leaflets and triggers the formation of calcium deposits – this process is what experts call calcification. Researchers at Fraunhofer IKTS are looking to stop these deposits from forming with new chemical pretreatments. They are working closely with the Institute of Applied Medical Engineer-ing at RWTH Aachen University and the Meshalkin National Medical Research Center in Novosibirsk, Russia.
“Although biological heart valves last for many years thanks to a special treatment process, signs of wear still appear and require these prostheses to be replaced after 10 to 15 years,” says Dr. Natalia Beshchasna, scientist at Fraunhofer IKTS. Deposits of calcium phosphate compounds negatively affect the mechanical properties of the material. The artificial valve becomes narrower, which impairs blood flow.
The prostheses are normally pretreated with glutaraldehyde. One of the purposes of this commonly used fixative is to stabilize the collagen scaffold of the prosthetic valve. To prevent or delay the calcification and degeneration process, Dr. Beshchasna and her partners are using new chemical compounds. In the trials, they selected pericardial tissue as a base material and stabilized it with molecules of active substance. Instead of conventional fixation with glutaraldehyde, they used diepoxide and bisphosphonate.
“Glutaraldehyde binds well to collagen, but not to elastin, which is also a component of pericardial tissue. That is why alternatives are being sought, and we have decided to use diepoxide,” explains the engineer. The cross-linking was carried out with and with-out adding bisphosphonates, which are medications that affect bone metabolism and are used to treat osteoporosis, for example.
Great potential for diepoxides and bisphosphonates
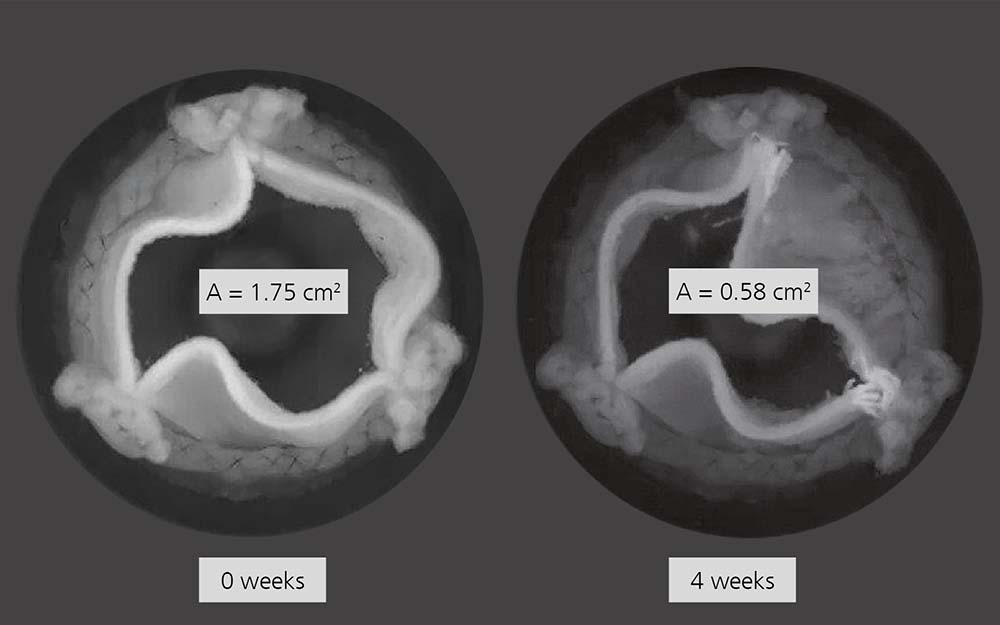
First of all, the tissue samples were prepared for three weeks with glutaraldehyde, diepoxide, diepoxide plus bisphosponate and diepoxide plus the mild preservative optiphen. This gave the tissue samples new properties. A four-week calcification test was then carried out to test the effects of the above-mentioned preparation under accelerated laboratory conditions. The pH of the solutions was buffered and matched that of human blood plasma. “We chemically pretreated a total of eight heart valves in different ways with four different solutions and analyzed them using conventional pro-cesses, such as scanning electron microscopy, Raman spectroscopy and microcomputer tomography, to determine which tissue treatment process works best against the long-term complication of calcification,” says the researcher. The results of the in-vitro test pointed to diepoxides and bisphosphonates as a highly promising alternative to glutar-aldehyde thanks to their excellent tissue fixation properties. The researchers see great potential for this combined treatment. “Pericardial tissue tends to bind calcium ions, which in turn bind phosphate ions, thus encouraging calcification of the prosthetic heart valve. Diepoxides and bisphosphonates can counteract this long-term complica-tion and prevent the reaction between calcium ions and phosphate ions,” says Beshchasna.
The next step is to confirm these promising results in further in-vitro and in-vivo tests and in clinical experiments. “So far, the perfect prosthetic valve has not been con-structed. We hope that our new chemical pretreatment will bring us one step closer to that holy grail.”